Search
- Page Path
- HOME > Search
Case Reports
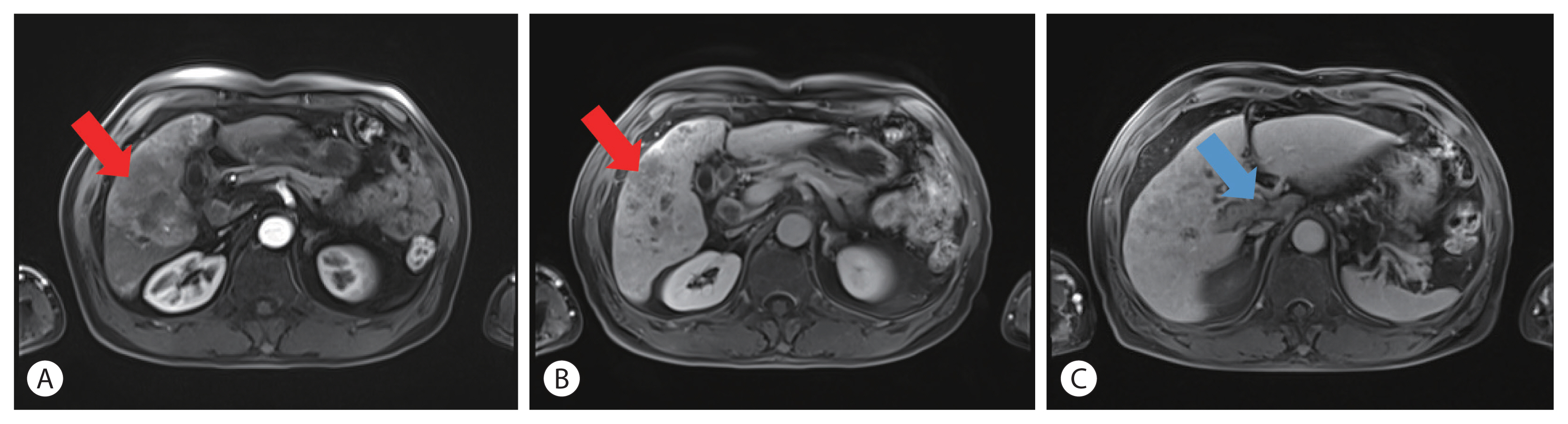
- A case report of a patient presented with skin ulcer after treatment of lenvatinib
- Serin Cha, Dong Woo Kim, Jung Wan Choe, Tae Hyung Kim, Seung Young Kim, Jong Jin Hyun, Sung Woo Jung, Ja Seol Koo, Young Kul Jung, Hyung Joon Yim
- J Liver Cancer. 2021;21(2):194-198. Published online September 30, 2021
- DOI: https://doi.org/10.17998/jlc.2021.09.20
- 3,312 Views
- 78 Downloads
- 1 Citation
-
 Abstract
Abstract
 PDF
PDF - A 60-year-old man diagnosed with unresectable hepatocellular carcinoma (HCC) presented to the hospital with pain in the perineal region. He had been taking lenvatinib every day for 2 months after he was diagnosed with HCC with metastases to the lymph node, small bowel mesentery, and retroperitoneal space. Enhanced abdominal computed tomography revealed mild elevation in intensity in the perineal subcutaneous tissue with subcutaneous emphysema. The patient was diagnosed with Common Terminology Criteria for Adverse Events grade 3, skin ulceration of stage IV with full-thickness skin loss and tissue necrosis in the muscular layer. The patient was taken off the medication with prescription of antibiotics, and after 3 weeks, the skin has fully recovered. This is the first report of an HCC patient who presented with a skin ulceration of stage IV after lenvatinib treatment. We recommend stopping the medication immediately and changing to alternative treatments with appropriate supportive care.
-
Citations
Citations to this article as recorded by- Multiple lenvatinib‐associated skin ulcers: A case report and literature review
Soo Hyun Jeon, Woo Jin Lee, Chong Hyun Won, Sung Eun Chang, Mi Woo Lee, Joon Min Jung
Australasian Journal of Dermatology.2023;[Epub] CrossRef
- Multiple lenvatinib‐associated skin ulcers: A case report and literature review

- A Case of Hepatocellular Carcinoma with Tumor Thrombus in Inferior Vena Cava and Right Atrium
- Hyun Jung Lee, Hyung Joon Yim, Hwan Hoon Chung, Seung Hwa Lee, Hae Rim Kim, Jong Jin Hyun, Sung Woo Jung, Ja Seol Koo, Sang Woo Lee, Jai Hyun Choi
- Journal of the Korean Liver Cancer Study Group. 2012;12(2):141-145. Published online September 30, 2012
- 607 Views
- 2 Downloads
-
 Abstract
Abstract
 PDF
PDF - In patients with advanced hepatocellular carcinoma (HCC), tumor thrombus in inferior vena cava (IVC) and right atrium (RA) are not uncommon findings and are usually associated with extremely poor outcome. Although aggressive surgical interventions such as extracorporeal circulation and tumor excision have been performed, the reported results were still unsatisfactory. Herein, we report the favorable result of combined treatment with radiation therapy and transarterial chemoembolization in a patient with advanced HCC with extensive tumor thrombus through the IVC into the RA. In conclusion, noninvasive combined modalities, such as transarterial chemoembolization and radiation therapy may sometimes provide effective palliation for patients with far advanced HCC with IVC/RA tumor thrombus and who are not candidates for alternative treatment options.

- A Case of Successful Treatment of Hepatocellular Carcinoma with a Pulmonary Metastasis by Combining Pulmonary Wedge Resection and Sorafenib
- Sun Jae Lee, Hyung Joon Yim, Hwan Hoon Chung, Hae Rim Kim, Eileen L. Yoon, Jong Jin Hyun, Sung Woo Jung, Ja Seol Koo, Rok Son Choung, Sang Woo Lee, Jai Hyun Choi
- Journal of the Korean Liver Cancer Study Group. 2012;12(1):67-70. Published online February 28, 2012
- 584 Views
- 1 Download
-
 Abstract
Abstract
 PDF
PDF - 35-year-old female patient was diagnosed with hepatocellular carcinoma and underwent hepatic resection. 12 months after hepatic resection, serum AFP rose (119.6 ng/mL) but no definite recurrence was found on imaging modalities. 30 months after hepatic resection, serum AFP rose up to 1008.5 ng/mL and metastatic nodule was found in right lower lung in chest CT. Video assisted thoracoscopic wedge resection was performed and 400 mg/day of sorafenib was intiated. Serum AFP returned to normal range after 2 months of pulmonary resection. No evidence of recurrence is noted after 30 months of pulmonary resection. We think that pulmonary resection plus sorafenib combination therapy resulted in favorable treatment outcome in this patient.

- A Case of Aggressive Treatment with Transarterial Embolization Using Drug-Eluting Beads for Hepatocellular Carcinoma in Decompensated Liver Cirrhosis Patient
- Eileen L. Yoon, Hyung Joon Yim, Hwan Hoon Chung, Seung Hwa Lee, Hae Rim Kim, Jong Jin Hyun, Sung Woo Jung, Ja Seol Koo, Sang Woo Lee, Jai Hyun Choi
- Journal of the Korean Liver Cancer Study Group. 2011;11(2):190-194. Published online September 30, 2011
- 542 Views
- 0 Download
-
 Abstract
Abstract
 PDF
PDF - Conventional transarterical chemoembolization (TACE) is the first-line treatment for patients with intermediate stage of hepatocellular carcinoma (HCC). However, irreversible liver failure after the procedure is one of the most feared complications and therefore, decompensated Child-Pugh C patients may not be the indication of the conventional TACE. Drug-eluting beads loaded with doxorubicin is a novel drug delivery embolization system and reported to have non inferior efficacy compared to conventional TACE. Also drug-eluting beads loaded with doxorubicin is associated with lower rates of acute liver failure after the procedure and lower rates of systemic toxicity of the chemotherapeutic agents. Herein, we report a case of aggressive treatment with transarterial embolization using drug-eluting beads loaded with doxorubicin for HCC in decompensated liver cirrhosis patient who was not eligible for conventional TACE treatment.


 E-submission
E-submission THE KOREAN LIVER CANCER ASSOCIATION
THE KOREAN LIVER CANCER ASSOCIATION

 First
First Prev
Prev



 Follow JLC on Twitter
Follow JLC on Twitter